#non-invasive-diagnostics
#non-invasive-diagnostics
[ follow ]
#ai-in-healthcare #healthcare #patient-safety #mental-health #chatgpt-health #breast-cancer-screening
from24/7 Wall St.
5 days ago5 Biotechs That Big Pharma Could Snap Up as Oncology M&A Heats Up
Incyte tops this list due to its rare combination of commercial scale, cash generation, and pipeline depth. The company posted FY2025 revenue of $5.14 billion, up 21.2% YoY, anchored by Jakafi generating $828.2 million in Q4 2025 alone (+7% YoY) and Opzelura delivering $207.3 million (+28% YoY). With $3.58 billion in cash and 14 pivotal clinical trials underway, Incyte offers an acquirer immediate revenue, margin expansion potential, and a deep oncology pipeline spanning KRASG12D, CDK2 inhibition, and mutCALR.
Venture
fromdesignboom | architecture & design magazine
6 days agobody agency and the ways wearable devices let people regain control of their physical forms
Body agency is a power returned after an incident took it away from the user's physical form, and some wearable devices and technologies have this exact goal in mind.
Wearables
Medicine
fromwww.scientificamerican.com
2 weeks agoNew early-warning alerts have doctors thinking it may be possible to repair a damaged kidney
Drug-induced acute kidney injury is common in hospitalized patients but often goes unrecognized because it causes no symptoms and damage occurs before creatinine levels rise enough to alert clinicians.
fromThe New Yorker
3 weeks agoDoctor Mike's Internet Medicine
If it continues to spread past the demarcation that we usually draw using a skin marker-we say Sharpie, but it's a skin marker-we say that this is spreading. Diagnosis: possible sepsis. Varshavski was not talking to the patient or to nursing staff. He was not even in a hospital. He was speaking into a camera in a two-bedroom apartment on the fifty-sixth floor of a building in Hell's Kitchen, in a makeshift studio where he records videos and his popular podcast.
Medicine
fromWIRED
1 month agoCuffless Blood Pressure Monitoring Is Coming. We Explain What It Is and How to Use It
Since 1990, the incidence of hypertension has increased globally, with up to one in three adults worldwide affected by it. Most of those people have no idea they have it. If people could diagnose and monitor hypertension at home, the World Health Organization estimates that up to 76 million lives could be saved with easy fixes, like stopping smoking or adjusting diet.
Health
fromTNW | Health-Tech
3 weeks agoCedars-Sinai's AI beats specialist models at reading heart scam
EchoPrime, a video-based vision-language model, analyses echocardiogram footage and generates a written report of cardiac form and function. Its findings were published in Nature (volume 650, pages 970-977) in February 2026, under the title 'Comprehensive echocardiogram evaluation with view primed vision language AI.'
Medicine
Healthcare
fromFortune
3 weeks agoMicrosoft launches Copilot Health, a dedicated space for personal health data and AI-driven insights | Fortune
Microsoft launched Copilot Health, an AI assistant feature that integrates and analyzes health data from wearables, electronic health records, and lab results to provide personalized health insights and provider recommendations.
Healthcare
fromHarvard Business Review
3 weeks agoHealthcare Uses Specialized Language. It Needs Specialized AI, Too.
Healthcare professionals across specialties use inconsistent terminology and communication styles, creating significant translation barriers that impede care coordination and data interoperability.
Healthcare
fromEngadget
3 weeks agoMicrosoft's Copilot Health can use AI to turn your fitness data and medical records 'into a coherent story'
Microsoft's Copilot Health aggregates medical records, fitness data, and health history to help patients prepare informed questions for their doctors, while explicitly not replacing professional medical advice.
fromNews Center
1 month agoAdvancing Preventive Care and Cardiovascular Risk Prediction Through Online Tools - News Center
As the Magerstadt Professor of Cardiovascular Epidemiology, Khan studies the epidemiology of risk for heart failure. Using population-based cohorts and large electronic health record data analyses, she performs mechanistic studies that may enhance risk prediction and identify novel therapeutic agents for the prevention and treatment of cardiovascular disease. Khan and her team have developed a tool to predict risk and prevent cardiovascular disease such as heart failure, stroke, arrhythmia, coronary artery disease and many other conditions.
Public health
Healthcare
fromTechRepublic
3 weeks agoAmazon Expands Health AI to Its Retail App, Offering Prime Members Free 24/7 Virtual Care
Amazon expands Health AI from its clinic app to Amazon.com and the Amazon app, positioning itself as an AI-powered healthcare entry point integrated with its retail ecosystem.
#healthcare-ai
Healthcare
fromwww.mercurynews.com
1 month agoAmazon bets on health care AI with tools for patients, doctors
Amazon Web Services launches Amazon Connect Health, an AI tool that automates medical documentation, billing codes, patient verification, and appointment scheduling to reduce healthcare administrative burden.
fromwww.bbc.com
2 months agoTrial launched to 'help spot health risks early'
Public health consultant Dr Ross Keat said supporting people earlier to make small preventative changes would make "a big difference later on". Some 3,500 people in the north of the island within that age bracket are eligible for the checks. The checks will be carried out by two pre-existing nurses that support GP staff and would not replace GP appointments, Keat explained, adding that the cost would be minimal and absorbed by Ramsey Group Practice.
Public health
Public health
fromwww.bbc.com
1 month agoPeriod blood test could offer less invasive alternative to cervical screening
Menstrual blood collected on a sanitary pad can detect cervical cancer signs, offering a potentially accurate, less invasive at-home screening alternative to clinician-collected cervical samples.
fromFast Company
2 months agoOpenAI enters the connected health space with ChatGPT Health
The feature, unveiled on Wednesday, creates a separate space within ChatGPT for health questions and discussions, where users can collect data from their connected health apps such as fitness apps and store their health files. Users can also connect to their electronic medical records through a partnership with b.well, OpenAI says. ChatGPT, then, does not have a direct integration with the MyChart patient records app from Epic, for example, but lets individual users make requests for their patient record data through integrations built by b.well.
Health
Public health
fromTechCrunch
2 months agoBiotics AI, Battlefield 2023, gains FDA approval for its AI-powered fetal ultrasound product | TechCrunch
Biotics AI received FDA clearance for computer-vision software that assesses fetal ultrasound quality, automates reporting, and aims to reduce prenatal diagnostic disparities.
fromBusiness Matters
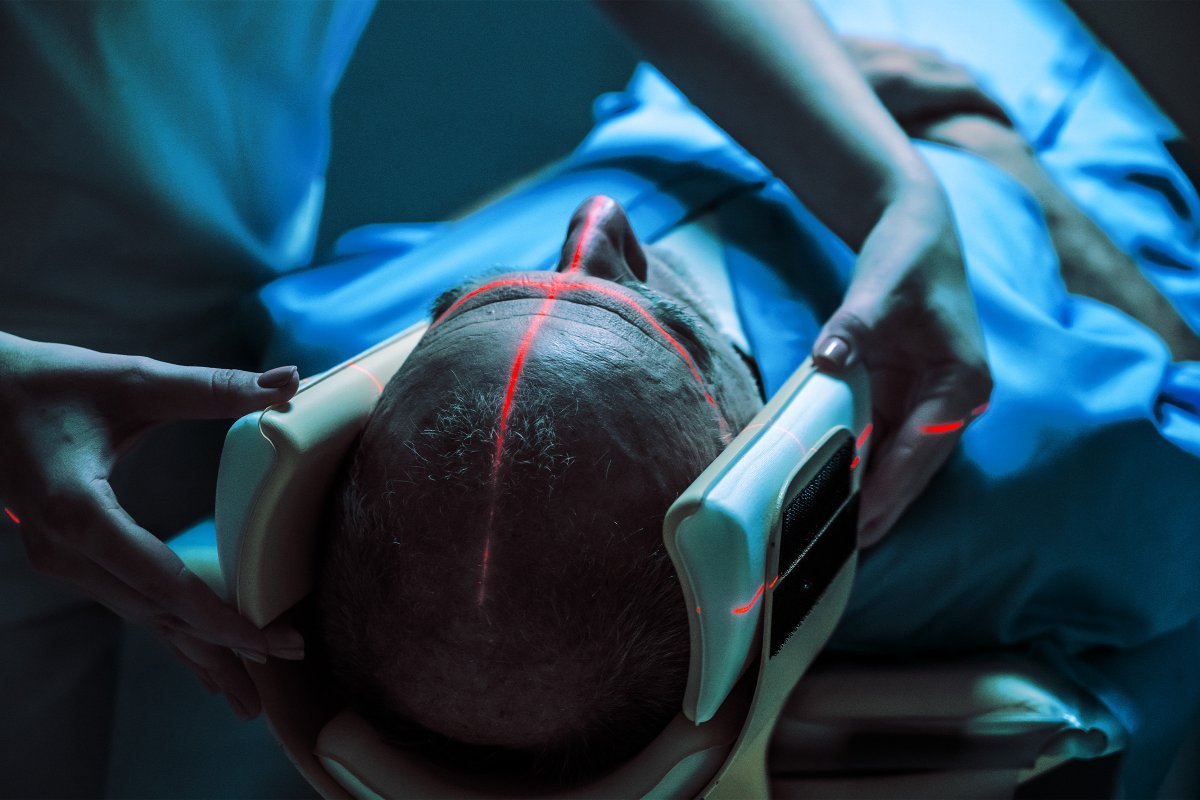
2 months agoThe Life Imaging Fla Story: Why Timing Matters in Modern Healthcare
After losing both of his parents to cancer, Tom set out to challenge a healthcare system that often waits for symptoms instead of identifying risk early. What began in Deerfield Beach, Florida, has grown into a multi-location preventative imaging company serving communities across the state. Life Imaging Fla focuses on preventative heart and full-body screenings. These services give people access to advanced imaging that is typically only approved once symptoms appear. The goal is straightforward: identify disease earlier, when people still have time, options, and control.
Medicine
fromFast Company
2 months agoConnected data will rescue healthcare
AI plays an important role-but not by fixing fragmented data on its own. The work of organizing, connecting, and interpreting healthcare information still belongs to people and the systems they build. Where AI helps is after that foundation is in place: by bringing the right information forward at the right time, reducing the effort it takes to find what matters, and supporting better decisions in the moment of care.
Medicine
fromPsychology Today
2 months agoMy Dad Got Sick-Doctors Dodged, AI Didn't
My dad was in the emergency room, short of breath, chest tight, upper back aching. He looked pale and confused. An ultrasound showed excess fluid between his lung and chest wall. "We'll drain it," a resident said, as if he were unclogging a sink. For the next five days, thick, red-tinged fluid filled a plastic container beside my dad's hospital bed. Doctors sent his cells for "staining," a way to identify cancer. But no one used that word.
Medicine
fromHarvard Gazette
2 months agoReal-world answers for patients running out of time - Harvard Gazette
But these studies typically require large numbers of patients, huge amounts of data, and thorough follow-ups, none of which comes easy or free. The upshot is fewer investigations into scenarios that are clinically important but unlikely to yield a profit for the firms funding them. Accordingly, researchers have been developing an option that uses real-world data from insurers to save patients from falling through the cracks.
Medicine
fromForbes
2 months agoWhy AI Chatbots Are Essential For Modern Medical Practices
The world of medical practice management is changing faster than ever, driven by two simultaneous forces: escalating patient expectations and crushing administrative complexity. In my years working with healthcare organizations, I've seen these challenges evolve from nuisances into crises. Research by Bain & Company found that 65% of healthcare consumers want more convenient experiences, and 70% want more responsiveness from providers. They want instant answers to routine questions, immediate scheduling access and minimal friction.
Healthcare
Medicine
fromwww.theguardian.com
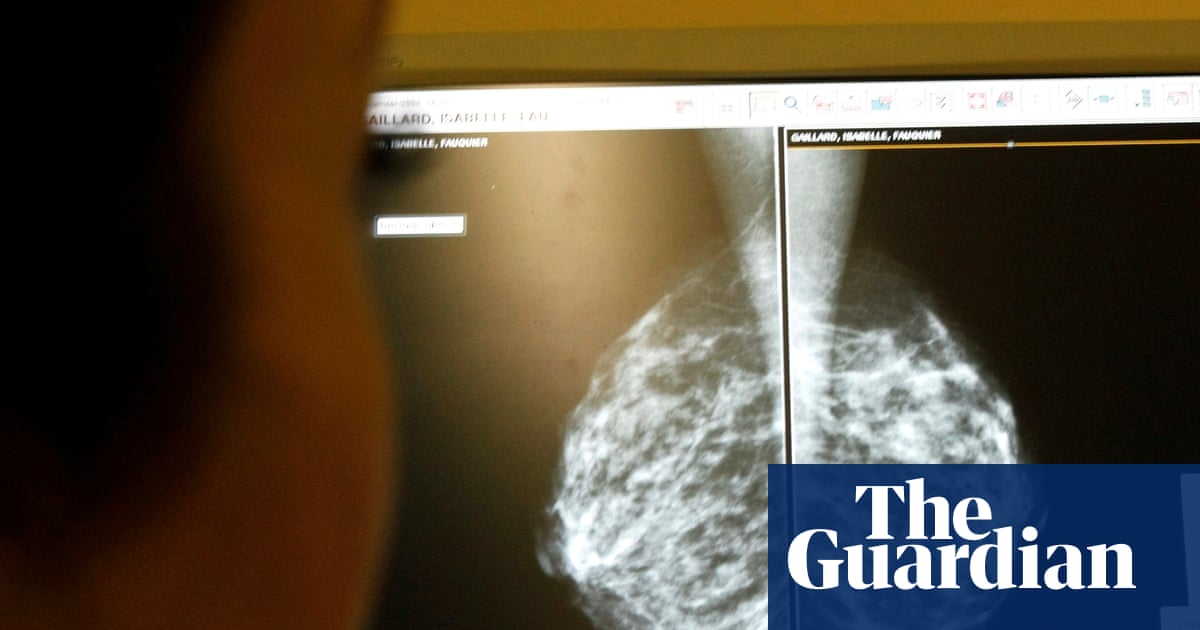
2 months agoSimple blood test can predict which breast cancer treatment will work best, study finds
A blood test measuring circulating tumour DNA predicts breast cancer treatment response before or within four weeks, enabling alternative therapies and avoiding ineffective drugs.
fromBusiness Matters
2 months agoThe Rise of Telemedicine: How Digital Health is Reshaping Medical Equipment Demand
Between March 2020 and March 2022, over 100 million telemedicine services were delivered to approximately 17 million Australians. The Australian government invested $409 million to make telehealth permanent, whilst the UK announced £600 million for digital health infrastructure in April 2025. Patient adoption is equally impressive: 60% find telemedicine more convenient than in-person appointments, 55% report higher satisfaction with teleconsultations, and 74% of millennials prefer virtual appointments for routine care. These aren't temporary shifts; they represent a fundamental transformation in healthcare delivery.
Healthcare
Healthcare
fromFortune
2 months agoWhen AI meets healthcare, how should payers react? | Fortune
AI can fully automate most transaction-oriented payer jobs, significantly boost knowledge and relationship work productivity, and replace many interpreter and doer roles, transforming payer operations and member services.
[ Load more ]